Part 2 of 3: The Human Gut Microbiome: The Gut-Brain Axis & Gut-Immune Axis
- Sentinel Health LLC

- Mar 26
- 8 min read
Updated: Mar 29
The GUT BRAIN-AXIS

The connection between the gut and the brain is more powerful than most people realize. This link, known as the gut brain axis, plays a crucial role in overall health, influencing everything from digestion to mood. When this connection is disrupted, it can lead to a range of physical and mental health problems. Understanding what the gut brain axis is, what harms it, and how to support it can help improve mental health & well-being.

What Is the Gut Brain Axis?
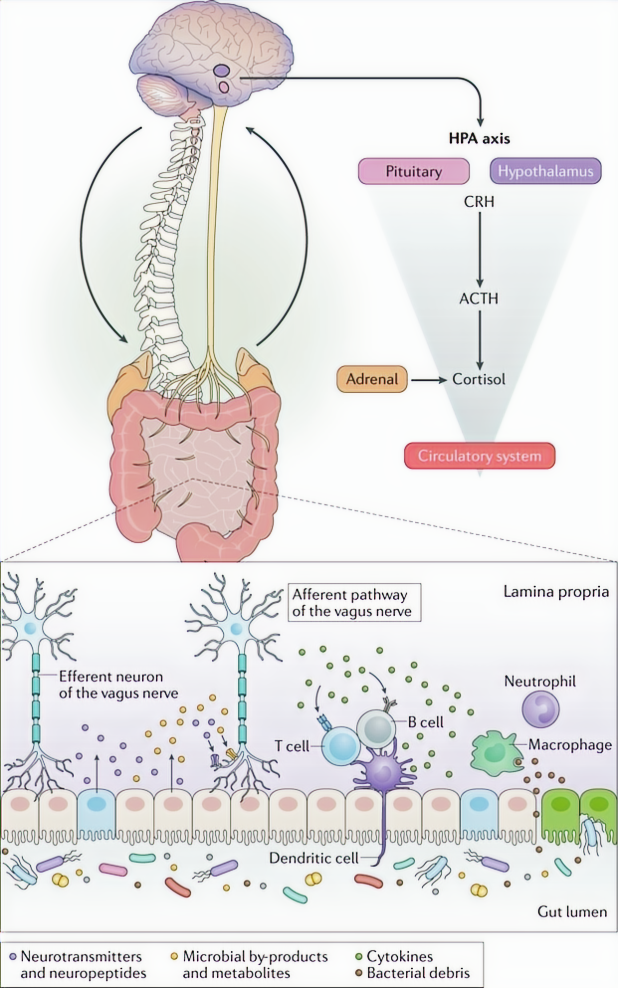
The gut brain axis is a two-way communication system between the gastrointestinal tract and the brain. This system involves nerves, hormones, and immune signals that allow the gut and brain to influence each other. The vagus nerve is a major pathway in this communication, sending signals from the gut to the brain and vice versa. The vagus nerve, also known as cranial nerve X, is the longest part of the autonomic nervous system, linking the brainstem to the heart, lungs, and digestive system. It serves as a main "rest and digest" controller, managing involuntary functions such as heart rate, digestion, and immune responses, and is crucial in reducing inflammation.
The gut contains trillions of bacteria, collectively called the gut microbiota. These bacteria produce chemicals that affect brain function and mood. For example, some gut bacteria produce neurotransmitters like serotonin, which plays a key role in regulating mood and anxiety.
This axis helps regulate digestion, immune response, and even emotional health. When it works well, it supports a balanced mood, good digestion, and strong immunity.
Neurotransmitters Produced by Gut Microbiota
The gut microbiota plays a significant role in the production of various neurotransmitters, which can influence brain function and behavior. Gut bacteria can metabolize dietary amino acids and other nutrients to produce neurotransmitters which then interact with your endocrine cells, By doing so, it influences the secretion of hormones that regulate neurotransmitter synthesis.
1. Serotonin
- Approximately 90% of the body's serotonin is produced in the gut. - Certain gut bacteria, such as *Escherichia coli*, can synthesize serotonin from tryptophan.
2. Gamma-Aminobutyric Acid (GABA)
- GABA is an inhibitory neurotransmitter that helps regulate neuronal excitability. - Some gut bacteria, including *Lactobacillus* and *Bifidobacterium*, have been shown to produce GABA.
3. Dopamine
- Dopamine is involved in reward and pleasure pathways in the brain. - Certain gut bacteria can produce dopamine, although the exact mechanisms are still being studied.
4. Norepinephrine
- Norepinephrine plays a role in the body's stress response. - Some studies suggest that gut microbiota may influence norepinephrine levels, although direct production by gut bacteria is less understood.
5. Acetylcholine
- Acetylcholine is critical for memory and muscle control. - Gut microbiota can impact the production of precursors necessary for acetylcholine synthesis.
What Damages the Gut Brain Axis?
Several factors can disrupt the gut brain axis, leading to imbalances in both gut and brain health:
Poor Diet
Diets high in processed foods, sugar, and unhealthy fats can harm the gut microbiota. Lack of fiber reduces the growth of beneficial bacteria.
Chronic Stress
Stress triggers the release of hormones that affect gut function and can alter the gut microbiome. This creates a feedback loop that worsens stress and gut health.
Antibiotics and Medications
While antibiotics fight infections, they also kill beneficial gut bacteria. Long-term or frequent use can lead to lasting imbalances.
Infections and Inflammation
Gut infections or chronic inflammation can damage the lining of the gut, affecting its communication with the brain.
Lack of Sleep and Sedentary Lifestyle
Poor sleep and inactivity negatively impact the gut microbiome and brain function.
When these factors persist, they can cause the gut brain axis to malfunction, leading to symptoms like digestive issues, mood disorders, and cognitive problems.
Effects of Damage to the Gut Brain Axis
Damage to this axis can show up in many ways, often affecting both physical and mental health:
Digestive Problems
Conditions such as irritable bowel syndrome (IBS), bloating, constipation, and diarrhea often relate to gut brain axis dysfunction.
Mood & Neuropsychiatric Disorders
Imbalances in gut bacteria and disrupted communication between the gut and brain have been associated with anxiety, depression, stress-related disorders, and autistic spectrum disorders.
Cognitive Issues
Problems with memory, focus, and mental clarity can arise when the gut brain axis is impaired.
Immune Dysregulation
Since much of the immune system is in the gut, damage can lead to increased inflammation and autoimmune conditions.
Sleep Disturbances
Poor gut health can interfere with sleep quality, which in turn worsens gut and brain function.
Neurodegenerative Disease
Although multifactorial, research has consistently identified patterns of impaired gut flora linked to Parkinson's, Alzheimer's disease, and Amyotrophic Lateral Sclerosis (ALS).

The GUT-IMMUNE AXIS
The gut microbiota plays a crucial role in maintaining our overall health, especially the immune system. When this delicate balance of microorganisms is disrupted, a condition known as dysbiosis occurs. Dysbiosis can significantly affect immune function, leading to increased susceptibility to infections, inflammation, and even autoimmune diseases. Understanding how gut microbiota influences immunity and the consequences of dysbiosis can help us make informed choices to support our health.

Gut Microbiota and Why It Matters for Immunity
These microbes perform essential functions such as:
Breaking down food and producing nutrients
Protecting against harmful pathogens
Training and regulating the immune system
The immune system relies on signals from the gut microbiota to distinguish between harmful invaders and harmless substances. This communication helps maintain immune tolerance and prevents unnecessary inflammation.
The Gut Microbiome and Immunity: Why Microbial Balance Matters for Immune Health
The human gastrointestinal tract is home to gut microbiome, which consists of bacteria, fungi, and viruses. This is a complex ecosystem that works in partnership with the body. These organisms play a fundamental role in digestion, metabolism, inflammation control, and immune regulation or dysregulation as is associated with autoimmune disorders such as Crohn's, Inflammatory Bowel Disease, Rheumatoid Arthritis, Hashimoto's, Sjogren's and Lupus. .
In fact, the majority of the immune system is located in the gut. Because of this close relationship, the balance of microorganisms within the intestinal tract strongly influences how effectively the immune system functions and how well the body can defend itself against infection.
The Gut Microbiota: The First Line of Defense
For a pathogen to successfully cause infection in the gastrointestinal tract, it must overcome three major protective systems: the gut microbiota, the intestinal barrier, and the mucosal immune system. Together, these systems form a highly integrated defense network designed to protect the body while maintaining tolerance toward beneficial microbes and harmless substances such as food. The gut microbiota acts as a protective biological barrier against invading pathogens. Beneficial microbes occupy ecological niches within the gut, competing with harmful organisms for nutrients and space. This protective mechanism is known as colonization resistance.
When healthy microbial communities are present, pathogens have difficulty establishing themselves in the intestinal environment. Beneficial bacteria also produce antimicrobial compounds and signaling molecules that further limit pathogen growth.
Microbial populations also communicate to monitor their population density and coordinate behaviors such as adherence, movement, and production of protective substances.

However, the microbial ecosystem is highly sensitive to environmental influences. Diet, stress, medications, aging, environmental toxins, and especially antibiotics can alter microbial composition. When the balance of beneficial and harmful organisms becomes disrupted, dysbiosis occurs and the microbiome can weaken. Opportunistic microbes may then gain the ability to grow, colonize, and trigger inflammation.
The Intestinal Barrier: A Critical Protective Shield
The second major defense system is the intestinal epithelial barrier, a single layer of specialized cells that separates the contents of the gut from the bloodstream and underlying tissues. These cells are tightly connected by protein structures known as tight junctions, which regulate what substances can pass through the intestinal wall.
Above the epithelial layer sits a protective mucus barrier that helps prevent microbes from directly contacting intestinal cells. This mucus also serves as a reservoir for protective immune molecules such as secretory IgA antibodies and antimicrobial peptides.
Together, the epithelial cells and mucus layer form a physical and biochemical shield that helps prevent pathogens from entering the body. However, this barrier is dynamic and can be disrupted by toxins produced by certain bacteria, inflammatory processes, or changes in the microbiome. When barrier integrity is compromised, microbial fragments and toxins may cross into the bloodstream, triggering immune activation and systemic inflammation.
The Gut Immune System: Constant Surveillance
The third major defense is the intestinal immune system, which works continuously to monitor interactions between microbes and host tissues.
The immune system is composed of two main branches:
Innate immunity, which provides rapid, nonspecific defense mechanisms such as antimicrobial peptides, immune cells, and inflammatory signaling.
Adaptive immunity, which provides targeted protection through specialized immune cells including T lymphocytes and B lymphocytes. T cells help coordinate immune responses and eliminate infected cells, while B cells produce antibodies that recognize specific pathogens.
Within the intestine, immune cells constantly sample microbial signals and determine whether a response is necessary. This process depends on specialized receptors called pattern-recognition receptors, which detect microbial structures and activate immune signaling pathways when needed.
Maintaining balance is essential. Too little immune activity may allow infection to develop, while excessive activation can lead to chronic inflammation or autoimmune disease.
Microbial Metabolites
One of the most important ways the microbiome influences immunity is through the production of microbial metabolites—biologically active compounds created when gut microbes process dietary nutrients.
Among the most studied of these metabolites are short-chain fatty acids (SCFAs) produced when gut bacteria ferment dietary fiber.
---SCFAs and how to support them with diet will be discussed further in a later post. ---
SCFAs support immune health in several ways:
• Strengthening the intestinal barrier• Stimulating mucus production• Enhancing antimicrobial peptide production• Promoting regulatory immune cells that reduce excessive inflammation• Supporting repair and regeneration of intestinal cells
Other microbial metabolites are produced from amino acids such as tryptophan. These compounds activate cellular receptors that regulate immune responses and maintain intestinal homeostasis. When dysbiosis occurs, the production of these beneficial metabolites often declines, contributing to impaired immune regulation and increased inflammation.

What Can Help Restore Balance?
Supporting the gut-brain axis & the gut-immune axis, involves lifestyle changes that promote a healthy gut microbiome and reduce stress on the system. Here are practical ways to restore balance:
Eat a Gut-Friendly Diet - More detailed information to come in Part 3
Feed beneficial gut bacteria. Foods that provide the fuel needed for beneficial bacteria to produce protective metabolites like short-chain fatty acids. Whole foods rich in fiber, such as fruits, vegetables, legumes, and whole grains.
Include fermented foods when tolerated. Foods such as yogurt, kefir, sauerkraut, and kimchi can introduce beneficial microbes that support microbial diversity.
Limit highly processed foods and excess sugar.Highly refined diets can disrupt microbial balance and promote growth of less beneficial organisms.
Manage Stress
Practices like meditation, deep breathing, yoga, or regular physical activity can reduce stress hormones and improve gut brain communication. Chronic stress and sleep disruption have measurable effects on the gut microbiome and immune regulation.
Limit Antibiotic Use
Use antibiotics only when necessary and under medical guidance. During and after antibiotic treatment, support gut health with probiotics and prebiotic foods for at least 2 weeks following antibiotics. If you are immune compromised, discuss the use of prebiotic and probiotics supplement with your provider.
Get Quality Sleep
Aim for 7-9 hours of restful sleep each night. Good sleep supports both brain, immune and gut health.
Stay Active
Regular exercise promotes a diverse gut microbiome, improving neurotransmitter production that impact mood and cognitive function and immune regulation..
Stay Hydrated
Drinking enough water supports digestion and overall gut function.
Probiotics and Prebiotics
Foods are the optimal way to enhance gut flora balance, but certain supplements can be beneficial in some situations. To avoid further disruption of the microbiota, it's advisable to consult a healthcare provider to identify the most suitable supplements.
General Recommendations:
Focus on long-term gut health. Improving microbial diversity and intestinal barrier function supports not only digestive health but also immune resilience, mental health, healthy aging and overall well-being.
The Functional Medicine Perspective

The functional medicine perspective looks for the underlying cause of the disease, not just managing the symptoms. The gut microbiome represents over all health and immune function. A healthy microbiome is an important part of treating most disease and common conditions, The idea is disease and illness prevention. Rather than focusing only on treating infections or inflammatory disease, functional medicine attempts to prevent the process from occurring in the first place. In cases where the disease or illness has already manifested itself, attention is placed on supporting microbial balance and intestinal barrier integrity in conjunction with managing the current disease state.

Fortunately, restoring balance is possible through
diet, stress management, sleep, and lifestyle adjustments.
More to come in the next blog -Part 3- on key changes
you can make to take control of your health.



